The American Headache Society's latest guidance recommends CGRP therapies as a first-line treatment for preventing migraine.
SIGNS YOUR MIGRAINE TREATMENT STOPPED WORKING — AND WHAT TO DO IF IT DOES
SIGNS YOUR MIGRAINE TREATMENT STOPPED WORKING — AND WHAT TO DO IF IT DOES
July 8, 2020
Karyn Repinski
Migraine disease can’t be cured, but pain-relieving medication (also known as “acute” or “abortive” treatment) often goes a long way toward stopping the progression of an attack. Sometimes, though, a treatment regimen that has been working well begins to fall short. It may take longer to work. You may find yourself needing repeated or increased doses to obtain a similar effect. Or maybe the medication just stops providing relief altogether.
Unfortunately, this loss of medication efficacy — the technical term is tachyphylaxis — is not uncommon. “I see it all the time in my practice,” says Merle Diamond, MD, president and managing director of the Diamond Headache Clinic in Chicago, and a board member of the National Headache Foundation.
Why Migraine Medication Stops Working
It’s not clear why medication becomes ineffective, reports neurologist Noah Rosen, MD, director of Northwell Headache Center in Great Neck, New York. “It may be related to a higher frequency of use, individual variability, or characteristics of the medication itself.” For instance, some medications have higher rates of migraine resolution and are more likely to provide 24-hour relief, whereas partial treatment may lead to recurrence and eventual loss of efficacy.
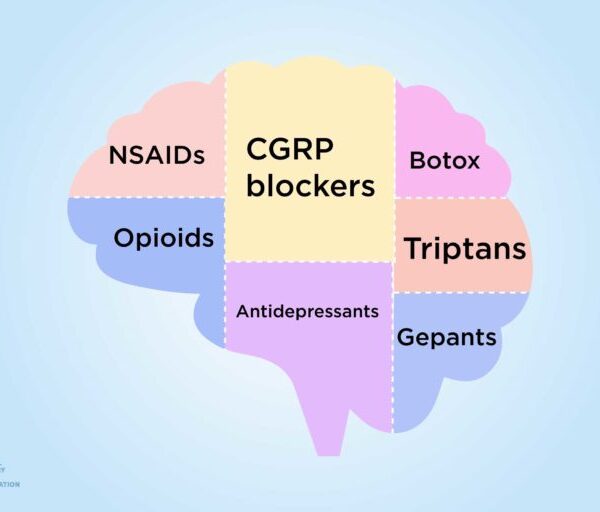
Acute medications with more specific effects, such as triptans, ditans, and gepants — all of which act on receptors in the brain — may have a greater likelihood of stopping migraine attacks and a lower chance of tachyphylaxis than non-specific migraine treatments like nonsteroidal anti-inflammatory drugs (NSAIDs), opiates, or barbiturates, says Dr. Rosen. “This is part of the reason it’s good to have an appropriate diagnosis, a good abortive strategy, and good communication with a health care provider to adjust meds as needed.”
When it comes to adjusting medications, a commonly suggested strategy is to try another medication within the same category when your current treatment stops working — for instance, giving one of the other six triptans that are available a shot if the one you’re taking begins to fail.
Unfortunately, there isn’t great evidence to show that this course of action is effective, says Dr. Rosen. Instead, he advises that “it may be worth trying other classes of acute medications, now that we have more options than ever before.”
What to Know Before You Switch Medication
Before you try another type of medication, however, there are a few things to consider about the medication you’re currently taking:
Are you taking it soon enough?
Waiting to treat your migraine can make it more difficult to respond to the medication. “You have to take the medicine as early in the attack as possible to get the desired impact, which is no pain in two hours and the ability to restore normal function without the headache coming back,” says Dr. Diamond, who’s a migraine patient herself. If you take the medication late, its effect may not kick in at all, or may kick in partially, but the head pain and other symptoms can remain. “That means you have to re-dose, which in turn can lower your threshold for your next migraine attack,” says Dr. Diamond.
Are you taking it too often?
Medication overuse can affect people who get migraine attacks, which can lead to shorter and shorter periods of pain relief. To avoid medication-overuse headaches (or “rebound headaches”), NSAIDs like aspirin and ibuprofen should not be used on more than 14 days a month. Drugs in the triptan family — often considered the gold standard medication for acute migraine treatment — should not be used on more than nine days a month.
The recently FDA-approved group of acute medications known as gepants — ubrogepant (Umbrelvy) and rimegepant (Nurtec) are the first two to become available — have a longer half-life than triptans, so medication overuse may not be an issue with them, says Dr. Diamond. Gepants are a type of medication that provides an acute treatment option for migraine patients who don’t respond to triptans or can’t safely take them due to cardiovascular risk factors.
In some studies, the daily use of gepants actually reduced the frequency of migraine attacks.
Are you taking the correct dosage?
“Another thing to pay attention to if you’re getting resistance to acute medication is dosage — I still occasionally see people who are given under-therapeutic doses of their triptans,” says Dr. Diamond. “For example, I’d say virtually everyone I know who takes sumatriptan orally needs 100 mg.” For all of the triptans, Dr. Diamond says very few people respond as well to lower doses that are available.
Why Keeping a Migraine Diary Is Key
To be sure you’re taking the right medication correctly, Dr. Diamond says, “keeping a migraine diary is super-important.” Whether you write it down in a journal or use a free app like Migraine Buddy, the goal is to track what medication you’re taking (including timing and dose) and how it’s affecting you so that your health care provider can help improve your treatment strategy.
Occasionally, patients find that the medication they’re taking to treat a migraine is the source of the problem. According to the American Migraine Foundation, because caffeine can trigger a migraine attack, taking an over-the-counter NSAID that contains caffeine can both not help your current headache and trigger another.
When to Consider Preventive Migraine Treatment
Sometimes you need to rethink how you’re taking your medication — and sometimes you may need to rethink what medication you’re taking. “Some patients take only acute medication because they don’t want to be on preventative medication,” for instance, due to potential side effects, says Dr. Diamond. “But if you take an acute medication and it works for a while and then stops and then you have to go to another one and that one stops, that is sometimes a signal — particularly if you have difficult-to-manage, frequent, or prolonged migraine attacks — that you need some prevention.”
Migraine preventative medication is considered when a patient has:
- Four to five migraine days a month with normal functioning
- Two to three migraine days a month with some impairment
- Two migraine days with severe impairment
Migraine preventative medication, which needs to be taken regularly and not just when a migraine strikes, can help reduce the frequency and severity of your attacks.
Options include drugs that have been used for years, such as beta blockers, antidepressants, and anti-seizure medications, as well as new drugs like CGRP blockers — Aimovig, Ajovy, Emgality, and Vyepti are currently available — that were specifically developed to prevent migraines.
Botox injections are also FDA-approved to prevent chronic migraine, which is defined as having at least 15 headaches a month at least four hours a day for more than three months.
Something to keep in mind about preventive treatments: Most studies on these medications lasted for six months or a year; some extended as far as three years.
“In real life, however, many people stay on preventive treatments far longer, although there is little evidence for continued efficacy,” says Dr. Rosen, who notes that recent studies of antidepressants have suggested little utility in longer-term treatment. In other words, sometimes people stay on preventive medication even though they may not actually be helping them anymore.
The upshot, he says: “It’s always good to have regular discussion with your health care provider to ensure that the efficacy has remained good and that the medication remains necessary.”
Be Mindful of Migraine Triggers
Many migraine patients can identify specific things — stress, sleep irregularities, hormones, diet, alcohol, light, and smells are common culprits — that make it more likely for them to experience a migraine attack. “Migraine can be challenging to treat because there can be so many triggers,” says Dr. Diamond.
Regardless of what medication you’re on, it’s important to remember that managing or avoiding triggers through diet or environment can help increase the effectiveness of your treatment, says Dr. Diamond.
If you aren’t aware of your triggers, keeping a migraine diary can help you determine what’s setting them off. It often takes a combination of triggers, such as having a glass of wine when you’re under a lot of stress, to provoke an attack. But once a pattern emerges, it should be easier to avoid things that trigger your migraines.
Interview with Merle Diamond, MD, president and managing director of the Diamond Headache Clinic in Chicago, and a board member of the National Headache Foundation
Interview with Noah Rosen, MD, director of Northwell Headache Center in Great Neck, New York
What to Do When Migraine Treatment Fails? American Migraine Foundation. May 10, 2018. https://americanmigrainefoundation.org/resource-library/what-to-do-when-migraine-treatment-fails.
If you enjoyed reading this article, you’ll love what our video has to offer.
SUBSCRIBE TO GHLF
RELATED POST AND PAGES
_
Was this article helpful?
YesNo





This Post Has 0 Comments